.png)
Chronic obstructive pulmonary disease (COPD) is one of the most prevalent lung conditions, affecting more than 328 million people around the world and an estimated 16 million people in the United States alone.
Despite how common COPD is, it’s often overshadowed by other chronic illnesses like lung cancer, heart disease, and diabetes. A report published by the EMBO Journal found that, while COPD results in about 300,000 deaths per year — nearly double that of lung cancer — it received less than a third of the funding.
While the inequity in COPD research funding can only be addressed through political and social advocacy, healthy lifestyle choices remain the best way to prevent and treat COPD. And in order to make healthy lifestyle choices, you need to stay educated about how your lungs work. There are a lot of things to consider depending on what stage of your life you’re in and whether or not you’ve already been diagnosed with COPD.
In this post, we’re going to address some key facts about aging and how it affects the prognosis of people with COPD and those who are at risk of contracting COPD. In the meantime, if you are interested in getting tested for COPD, be sure to consult your doctor immediately to start discussing your symptoms.
{{cta('fa8abc2a-1e88-4fa3-82fd-1cb5b9ed43b2','justifycenter')}}
COPD Takes Several Years to Develop
One of the main differences that sets COPD apart from lung cancer and other chronic illnesses is the rate at which it develops. According to MedicineNet, small cell lung cancer is known to develop extremely quickly and can often result in death within 6 months if it is left untreated.
COPD is very different from this because you’ll see the disease develop over several years or even decades rather than over months. While smoking immediately results in symptoms like coughing, wheezing, and breathlessness, it takes several years before medical professionals can actually associate these symptoms with COPD.

Another factor contributing to the rate of onset of COPD is how many cigarettes you smoke and how frequently you smoke. While researchers aren’t entirely sure what amount of cigarettes will cause COPD, they do agree that even just one cigarette can cause permanent damage to the body.
Many people consider themselves to be “social smokers” because they only smoke when they’re with friends. These people may feel better about their habit because they feel more in control of how much they smoke, but the truth is, they may be at just as high of a risk of contracting COPD as a chronic smoker.

Another risk of being a “social smoker” is that you’re being exposed to a lot more cigarette smoke than you realize. A common myth about smoking is that inhaling second-hand smoke is more dangerous than actually smoking. This is not the case, but it is still equally damaging to inhale second-hand smoke, so you should avoid hanging out around people who smoke.
The key takeaway from this is that your body isn’t going to give you any major warning signs that you have COPD. Long-term symptoms of COPD are similar to the short-term side-effects of smoking which will mask any serious underlying issues you’re facing. The difference, of course, is that the symptoms you experience from COPD are permanent. The best way to avoid COPD is to quit smoking immediately and visit your doctor.
Underdiagnosis and Misdiagnosis are Common in COPD
Diagnostic error is a much more common issue than many people realize. According to Improveddiagnosis.org, an estimated 12 million Americans experience an inaccurate diagnosis in their life, and between 40,000 to 80,000 people die each year as a result of diagnostic errors in hospitals.

These are startling numbers, but you may be surprised to find that people showing signs of respiratory illness are some of the most commonly affected by diagnostic errors. Like we discussed in a previous post, COPD is not always an easy condition to diagnose. Inconsistencies in testing procedures like spirometry can throw off results and miscommunications between doctors and their patients can contribute to this.
One of the most common diagnostic errors is COPD patients being diagnosed with asthma. According to a study published in the National Jewish Health Journal, more than half of COPD patients may be misdiagnosed with asthma. This is not surprising, as both conditions exhibit similar symptoms such as coughing, wheezing, and shortness of breath.

The biggest danger of being misdiagnosed for respiratory symptoms is that you will receive the wrong treatment plan. Asthma is most often treated with fast-acting inhaled medication like bronchodilators which help to open up the airways and prevent asthma attacks. However, COPD treatment is more involved and includes things like supplemental oxygen therapy, long-acting inhaled medication, pulmonary rehabilitation, and an improved diet.
Someone who was misdiagnosed with asthma may live for years without being correctly diagnosed or they may never be correctly diagnosed with COPD. Another way COPD can be misdiagnosed is if a patient is diagnosed with asthma when they’re young. If respiratory symptoms increase with age, they may dismiss them as asthma symptoms, and never seek professional help.

The best way to avoid a missed or delayed diagnosis for COPD is to ensure that you’re always honest and upfront about your symptoms. It’s not normal to have a cough or chest pain that lasts more than a few days and asthma does not necessarily get worse with age. Visit your doctor often and don’t be afraid to ask a lot of questions.
Younger Generations Could be Less Predisposed to COPD
Not all news surrounding chronic obstructive pulmonary disease is negative. You’ll be happy to know that younger generations may be far less predisposed to contracting COPD than their parents and grandparents. This is primarily due to changing regulations surrounding smoking and pollution, and more stigma surrounding smoking at a young age.
![]()
On July 1, 2006, the Colorado Clean Indoor Air Act went into effect which banned smoking in public indoor places. This law was updated in 2019 to include the following:
- E-cigarettes and vaping are now included in the ban
- Originally, smoking was not permitted within 15 feet of a public building; this has been extended to 25 feet
- Exemptions for smoking areas in airports and hotels have been removed
While other states have their own rules and regulations concerning smoking and vaping, generally speaking, the country is moving in the right direction when it comes to lowering the risk of future generations contracting COPD, lung cancer, and other chronic lung conditions.
Another factor to consider is the increased social stigma attached to smoking. In the past, smoking was seen as stylish or cool, but over time, public perception of smoking has changed significantly. A study done by UC San Francisco and Stanford University School of Medicine examined the adolescent perception of smoking in 2001 versus 2015 and found that it’s largely looked down upon.
![]()
This study found that 94 percent of students in 2015 and only 65 percent in 2001 intended not to smoke and that only 17 percent of students believed smoking made them look more mature in 2015, as opposed to 27 percent in 2001.
Changes to environmental regulations could also play a major role in reducing COPD predisposition in future generations. Researchers have found that air pollution like dust, exhaust, fumes, and chemicals can all contribute to the onset of COPD, both in smokers and non-smokers. So, as we see a push towards cleaner or fewer emissions, we should see a corresponding drop in COPD cases all across the country.
Alpha-1 Deficiency Could Lead to Earlier Onset of COPD
Alpha-1 antitrypsin (AAT) deficiency is a genetically transmitted disorder that increases someone’s likelihood of contracting COPD. It occurs when there is a lack of the protein alpha-1 antitrypsin in the blood which the lungs use to reduce inflammation and infection in the lungs. Abnormal genes affect the way that alpha-1 protein is created and excreted from the liver.

Contrary to common belief, alpha-1 deficiency does not cause COPD in and of itself. However, it does make your lungs more susceptible to factors that can cause COPD. In other words, if you have alpha-1 deficiency and you smoke or you’re exposed to high levels of air pollution, you’re more likely to contract COPD, and you’ll likely contract it more quickly than someone without the disorder.
One of the biggest dangers of alpha-1 deficiency is that it’s fairly uncommon with only 100,000 cases in the United States. What this means is that doctors don’t typically test for it and it’s usually only discovered if you happen to have blood drawn for some other reason. AAT plays an important role in breaking down an enzyme called neutrophil elastase which is part of the natural immune response in the lungs. In a healthy person, these enzymes are controlled and cause no threat to the lungs, but in someone with AAT deficiency, it can cause permanent and irreversible damage.
While rare, AAT deficiency simply reinforces the importance of getting tested as early as possible. There are many different treatment options for alpha-1 deficiency including augmentation therapy, which aims to infuse the missing protein directly into the patient’s blood. Other treatment options include vaccinations that prevent infections and an improved diet which promotes healthy lungs and liver.
COPD is Commonly Diagnosed in Late Adulthood
Even when COPD is diagnosed correctly, it’s usually only found in older adults. According to Healthline, of the 8.9 million Americans diagnosed with chronic bronchitis in 2016, 75 percent of them were over the age of 45. There are also stark gender differences with 5.9 million women receiving a diagnosis and only 3 million men receiving a diagnosis.

It’s estimated that about 40 percent of people with COPD have not yet been diagnosed. It’s safe to assume that many of these people are experiencing early stage 1 COPD and they are simply brushing off the symptoms as a sign of aging. However, it’s important to note that chronic coughing or wheezing are never symptoms of normal aging. COPD is often associated with recurring lung infections that can cause this.
No matter what age you’re diagnosed at, COPD treatment will look pretty similar. Since COPD is characterized by progressive lung inflammation and obstruction, your doctor’s primary goal will be to slow the rate of lung decline while simultaneously reduce your risk of exacerbation (a flare-up in your respiratory symptoms).

An improved diet is one of the primary treatments for COPD. Regardless of your age, your body needs a healthy balance of vitamins, minerals, and other nutrients in order to stay healthy. Your lungs depend on these in order to promote healthy blood flow, efficient breathing, and to help control inflammation which can cause chest pain and accelerate the progression of your disease.
Secondly, your doctor will likely set you up with a pulmonary rehabilitation routine. Think of this like a controlled exercise program that’s specifically designed to educate you about your lungs and how to train them for maximum efficiency. Of course, pulmonary rehabilitation will look different based on your age and what your physical abilities are. Ultimately, the goal isn’t to be an all-star athlete, it’s to keep your muscles in shape and improve your endurance so that you don’t feel out of breath so frequently.

Lastly, your doctor will look at medications such as supplemental oxygen, nebulizer therapy, and inhaled corticosteroids. Typically, patients with stage 1 or stage 2 COPD are instructed to use supplemental oxygen for several hours a day, whereas patients with more severe stage 3 or stage 4 COPD will likely need to use oxygen 24/7 in order to receive its full effects. Oxygen is effective at not only reducing COPD symptoms, but it can also reduce the likelihood that you will experience a COPD exacerbation. If you’re looking for an oxygen device for seniors, portable oxygen concentrators tend to be the best option because they offer the most freedom and independence.

A nebulizer is a small device that delivers medication as a mist that can be inhaled. Nebulizers are most often used by younger children or seniors who are not able to effectively time their breathing well enough to use an inhaler. They’re also much easier to use than oral medication which can be difficult to swallow. Some common drugs administered through nebulizer therapy include ipratropium bromide, cromolyn sodium, albuterol, levalbuterol, budesonide, and acetylcysteine.
{{cta('43b79c5e-6bd6-4f02-ac27-2d038d20c146','justifycenter')}}
Managing COPD is More Difficult in Seniors
Potentially the most urgent age-related issue associated with COPD is its effects on seniors. Old age is already associated with a number of issues such as joint pain, muscle pain, fatigue, and chronic health conditions which can only make coping with COPD more difficult. Generally speaking, the older your age, the shorter your life expectancy with COPD will be.
Joint and Muscle Pain
Chronic pain in the joints and muscles is more common than you may think. According to WebMD, about one in three adults have experienced joint pain in the past 30 days and this only gets worse with age. Joint and muscle pain can be brought on by an injury or one of many chronic underlying conditions such as osteoporosis, osteoarthritis, gout, or bursitis.

One of the ways these issues can affect COPD patients, in particular, is through reduced mobility. COPD is considered a debilitating disease meaning it makes you weak and feeble. Osteoporosis, a condition that results in weak, fragile bones, can contribute to COPD symptoms like rib or chest pain.
Respiratory Infections
Influenza and the common cold are two of the most common infections in the world. And as of late, we’ve been introduced to a new type of viral respiratory infection: COVID-19. While anyone can contract these illnesses, they’re more common in older adults and they can be far more deadly, especially when they’re combined with chronic diseases like COPD. According to the American Lung Association, you’re 7.7 times more likely to contract pneumococcal pneumonia (a type of bacterial pneumonia) if you have COPD and you’re over the age of 65.
Since bacterial infections are responsible for around 40 to 50 percent of all COPD exacerbations, it is imperative that you do everything you can to avoid acute illness. Cleaning your home regularly with natural and safe cleaners is a great place to start, and you should visit a doctor immediately if you experience any unusual symptoms.
COPD Comorbidities
A comorbidity is a condition that exists alongside another one. Some of the most common comorbidities of COPD include obstructive sleep apnea (OSA), pulmonary hypertension, coronary artery disease, and heart failure. Sometimes, comorbidities can be treated with COPD medication or therapies, but other times, they require a separate treatment plan in order to address the underlying issues.
.jpg)
Obstructive sleep apnea is common. According to sleepapnea.org, between 11 and 19 percent of COPD patients have it and almost half of all COPD patients experience some type of sleep difficulty. If this is the case, your doctor may advise that you use supplemental oxygen therapy, CPAP therapy, or both that night in order to promote restful sleep.
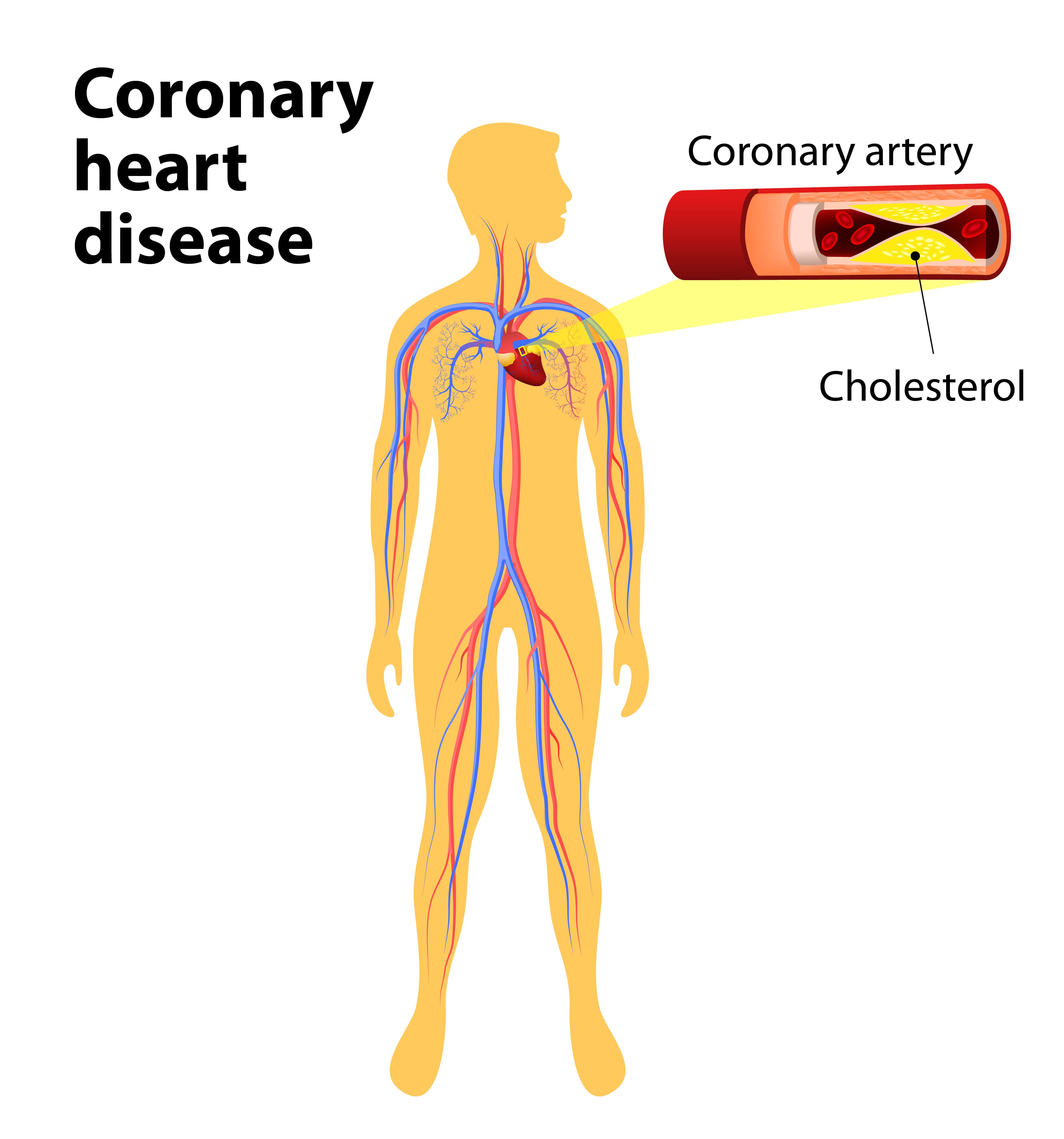
Coronary heart disease is a condition that’s usually caused by the build-up of plaque in the arteries of the heart causing them to narrow and blocking blood flow. Just like COPD, one of the main causes of coronary heart disease is smoking, so it’s not surprising that having chronic bronchitis will raise your risk of contracting it by about 50 percent. Other risk factors of coronary heart disease include high cholesterol, systemic hypertension, and a high body mass index (BMI).
Conclusion
Chronic obstructive pulmonary disease is one of the leading causes of mortality in the world; It’s also one of the most preventable illnesses in the world. Whether you’re a young adult or a senior, it’s important to always make good health decisions and to be more aware of how your lifestyle affects your lungs.
Age has a significant impact on your ability to prevent and treat COPD. Younger generations may be less likely to contract COPD because of the stigma associated with smoking and pollution. On the other hand, seniors with COPD will have a harder time managing their disease than a young person due to comorbidities and other issues caused by aging.
Regardless of your age, your doctor should be the first person you go to if you’re experiencing chronic symptoms. Coughing, wheezing, and chest pain are not normal signs of aging, so if they persist for more than a couple of days, you should schedule an appointment as soon as possible.

