
Do you ever wonder what is exactly happening to your body? What do these diagnoses mean for you and life as you know it?
{{cta('fa8abc2a-1e88-4fa3-82fd-1cb5b9ed43b2','justifycenter')}}
If so, you need to read this blog that explains bronchiectasis in depth. Bronchiectasis is a condition where the bronchial tubes of your lungs are permanently damaged, widened, and thickened. This is an important illness that we at LPT Medical take very seriously. When it comes to oxygen therapy and supplemental oxygen devices, we are your go to company that supplies the most effective, quiet, high-tech oxygen machines.
Bronchiectasis causes damage to people’s air passages. Bronchiectasis often happens as a result of COPD. In these cases, many people will require a portable oxygen concentrator in order to get the right amount of oxygen.

The damages bronchiectasis causes in the lungs also causes bacteria and mucus to build up and compile in the lungs. This results in frequent infections and blockages of the airways. That being said, in conjunction with oxygen therapy, bronchiectasis patients must also be prepared with a proper treatment plan that can mitigate infections and exacerbated symptoms.
There is a lot more to this disease than what meets the eye. The sections in this blog will explain bronchiectasis and everything you need to know about what it means for you moving forward.
COPD and Bronchiectasis Overview
Bronchiectasis and chronic obstructive pulmonary disease (COPD) are two chronic conditions that involve damage to the lungs and they often happen together. In many cases, people with both of these conditions need pulse flow oxygen or a continuous oxygen device. The ARYA Portable Oxygen Concentrator is an example of a pulse flow device that people can use day or night. The Respironics SimplyGo is a continuous flow device that is very popular.

If you have other questions about portable oxygen concentrators, call LPT Medical at 1+(800)-946-1201.

The causes and treatments for each differ slightly. It is common for COPD to cause bronchiectasis.
It is important for you to know the differences and similarities between bronchiectasis and COPD and how each condition is treated.
There’s no cure for bronchiectasis or COPD, but both are treatable. With the proper treatment, you can lessen symptoms and slow the progression of the disease from getting worse. Bronchiectasis is objectively more mild, and with treatment, you can actually live a fairly normal life with less invasive symptoms and treatments than what one would go through with COPD.
.png)
With bronchiectasis, flare-ups must be treated quickly to maintain oxygen flow to the rest of your body and prevent further lung damage.
Because this blog is more focused on bronchiectasis, we are not going to dive deep into the similarities and differences between COPD and bronchiectasis. We did find a very useful Healthline article that explains this comparison more. You can find that by clicking here: Understanding the Similarities and Differences Between Bronchiectasis and COPD.
The rest of this blog is going to explain the bronchiectasis diagnosis, the symptoms of bronchiectasis, risks associated with developing bronchiectasis, tips for living with bronchiectasis, and lastly the treatment and outlook for people with bronchiectasis.
Bronchiectasis Diagnosis Process
A chest computed tomography also known commonly as a CT scan is the typical test for diagnosing bronchiectasis. X-rays are less accurate in diagnosing bronchiectasis.
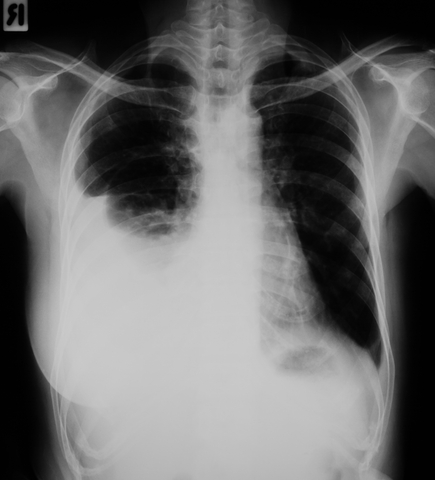
The CT scan is a painless test. It shows exact copies of your airways and other structures in your chest. A chest CT scan can show the extent and location of lung damage.
It is important during the diagnosis process, for your doctor to work with you to establish the cause of the bronchiectasis based on your history and physical exam findings. There are several causes that can cause or contribute to bronchiectasis.
Bronchiectasis is normally caused by your lungs becoming damaged and airways widening and becoming infected. This is why COPD often results in bronchiectasis. Sometimes, the cause of bronchiectasis is unknown.
You might be wondering— why is it important to know the cause of bronchiectasis? This is so that you and your healthcare team can effectively treat the underlying disorder to prevent the bronchiectasis from getting worse.
That being said, during your diagnosis process, you’ll want to know the underlying cause. Therefore, after your CT scan confirms you have bronchiectasis, you’ll then undergo laboratory and microbiologic testing and pulmonary function testing.
This evaluation will likely include:
- Complete blood count with differential
- Immunoglobulin levels (IgG, IgM, and IgA)
- Sputum culture to check for bacteria, mycobacteria, and fungi
- If your doctor suspects CF, they’ll order a sweat chloride test or genetic test.
Bronchiectasis Symptoms Explained
If you think you have bronchiectasis, you can monitor the sign and symptoms by researching what exactly bronchiectasis looks like. However, symptoms of bronchiectasis can take several months or even years to develop.

Some if the common symptoms include:
- chronic daily cough
- coughing up blood
- atypical sounds or wheezing in your chest with breathing
- shortness of breath
- chest pain
- coughing up large amounts of thick mucus every day
- weight loss
- fatigue
- change in the structure of your fingernails and toenails, known as clubbing
- frequent respiratory infections
If you’re experiencing any of these symptoms daily, you should contact a doctor. You can get a diagnosis and start treatment immediately to mitigate the progression and severity of the disease.
Risks and Developing Bronchiectasis
The risk of developing bronchiectasis increases as you get older. That being said, younger people can have it. Also, Women are more likely to have it than men, and women's experience with bronchiectasis also tends to be more severe.

Other health conditions that can put you at risk of having bronchiectasis include:
- Atypically functioning immune system
- Inflammatory bowel disease
- Autoimmune diseases like HIV
- COPD
- Allergic lung reaction to fungus
- Lung infections, such as whooping cough, pneumonia, or tuberculosis
Tips for Living with Bronchiectasis

Once you have bronchiectasis, there is no cure. This is a disease you will live with you the rest of your life. Therefore, you will need to learn how to live with the symptoms, treatments, and other conditions of the disease.
The bright side is that you CAN live with this disease. If you treat yourself properly, you can live a relatively normal life as you would without the disease!
Here are the basic tips you need to follow:
- Follow your bronchiectasis treatment plan.
- Take your medications as prescribed.
- Eat a healthy, well-balanced diet.
- Drink lots of water and other nonalcoholic beverages.
- Follow a gentle exercise routine.
- Practice good sleep hygiene.
- Get your annual flu shot.
- Get your COVID-19 vaccination and booster.
- Wash your hands.
- Avoid getting the common cold, flu, COVID and other illnesses.
- Perform breathing exercises and techniques.
- Maintain good posture.
- Relax and incorporate rest periods throughout your day.
- Do your more difficult tasks when your energy levels are highest.
Treatment for People with Bronchiectasis

So as we mentioned above in the first tip for living with bronchiectasis— You have to follow a strict treatment in order to live comfortably with bronchiectasis
Treating your bronchiectasis is important to help you manage the condition and daily life. Your main goal of treatment should be to keep infections manageable. So how do you do this?
Your treatment options for bronchiectasis include:
- Chest physiotherapy. Chest physiotherapy helps clear your lungs of mucus. This is a compression vest that gently pushes and releases your chest, creating the same effect as a cough. The purpose is to clear mucus from the walls of your bronchial tubes.
- Surgery. If there’s bleeding in your lung, or if the bronchiectasis is only in one part of your lung, you may need surgery to remove the affected area.
- Draining secretions. Another part of daily treatment involves draining the bronchial secretions, aided by gravity. A respiratory therapist can teach you techniques to aid in coughing up the excess mucus
- Treating underlying conditions. If conditions like immune disorders or COPD are causing your bronchiectasis, you will treat those conditions in order to mitigate bronchiectasis symptoms. Common treatments for COPD include oxygen therapy and pulmonary rehabilitation.
- Lifestyle changes. Things like exercise, eating a healthy diet, and drinking plenty of water may help improve the symptoms of bronchiectasis.
Outlook for People with Bronchiectasis

The outlook for people with bronchiectasis is dependent on the severity of the condition, how you treat the condition, and most importantly what is causing it.
Bronchiectasis affects 350,000 to 500,000 people in the U.S. Individuals with the non‐cystic fibrosis bronchiectasis overall have a positive outlook with treatment. That being said, severe bronchiectasis can be fatal.
Non‐cystic fibrosis bronchiectasis is a chronic lung condition in which the breathing tubes in the lungs, also known as airways or bronchi, become abnormally dilated and thickened over time. While there are many causes of bronchiectasis, damage to the airway by lung infection is the most common. These damaged airways can no longer effectively clear mucus and bacteria from the lungs.
Cystic fibrosis (CF) is a genetically inherited disorder that causes severe damage to the lungs, digestive system and other organs in the body. Cystic fibrosis affects approximately 30,000 children and adults in the United States and approximately 80,000 individuals worldwide.
Overview
One of the biggest and most important things when it comes to bronchiectasis is early diagnosis.
The earlier and faster you can begin treatment, the better it will be for managing the lung damage you already have and preventing it from getting worse.
Beyond early diagnosis, we hope that this article sheds light on bronchiectasis and how the disease will affect you and your daily life!
Please leave a comment or question if you enjoyed reading this blog, and share the link with friends, family, and followers to help others learn more about bronchiectasis.

