
Chronic obstructive pulmonary disease (COPD) is one of the leading respiratory diseases in the world in terms of morbidity and mortality. Around 65 million people have it, and many experts are expecting that number to grow over the next 50 years. One thing that’s unique about COPD is the fact that it develops very slowly over the course of many years. Because of this, many COPD patients are susceptible to complications that are as bad, or even worse than their underlying condition.
One of the most notable examples of this which often occurs in the later stages of COPD is heart disease. Since the heart and lungs work together to distribute oxygen throughout the body, impaired lung function can result in added strain on the heart. Over time this can cause serious complications like right-sided heart failure, heart attacks, and coronary artery disease.
{{cta('fa8abc2a-1e88-4fa3-82fd-1cb5b9ed43b2','justifycenter')}}
Fortunately, studies have shown that — by proactively managing your respiratory symptoms — you’ll significantly reduce your risk of experiencing complications from COPD. Treatments like oxygen therapy will reduce the workload on your heart and lungs and ensure that every organ in your body has the oxygen it needs to function properly. However, it’s still important to understand the complications of COPD so that you know what symptoms to look out for.
In the following sections, we’ll take a look at one of the lesser discussed COPD complications called pneumothorax, also known as a collapsed lung. If you have any questions about the content of this article, please address them in the comment section below. However, if you have questions about your COPD or treatment plan be sure to consult with your doctor. COPD is a complex disease, so something that works for one person may not work for another.
What is Pneumothorax?
“Pneumothorax” is the medical term used to describe a collapsed lung. This occurs when air enters the “pleural space” which is the area around your lungs. This disrupts the balance of pressure between the inside and outside of your lungs and can result in a collapse of the lung. Pneumothorax ranges in severity from mild to life-threatening. Mild pneumothorax often needs no medical attention and will heal over time.
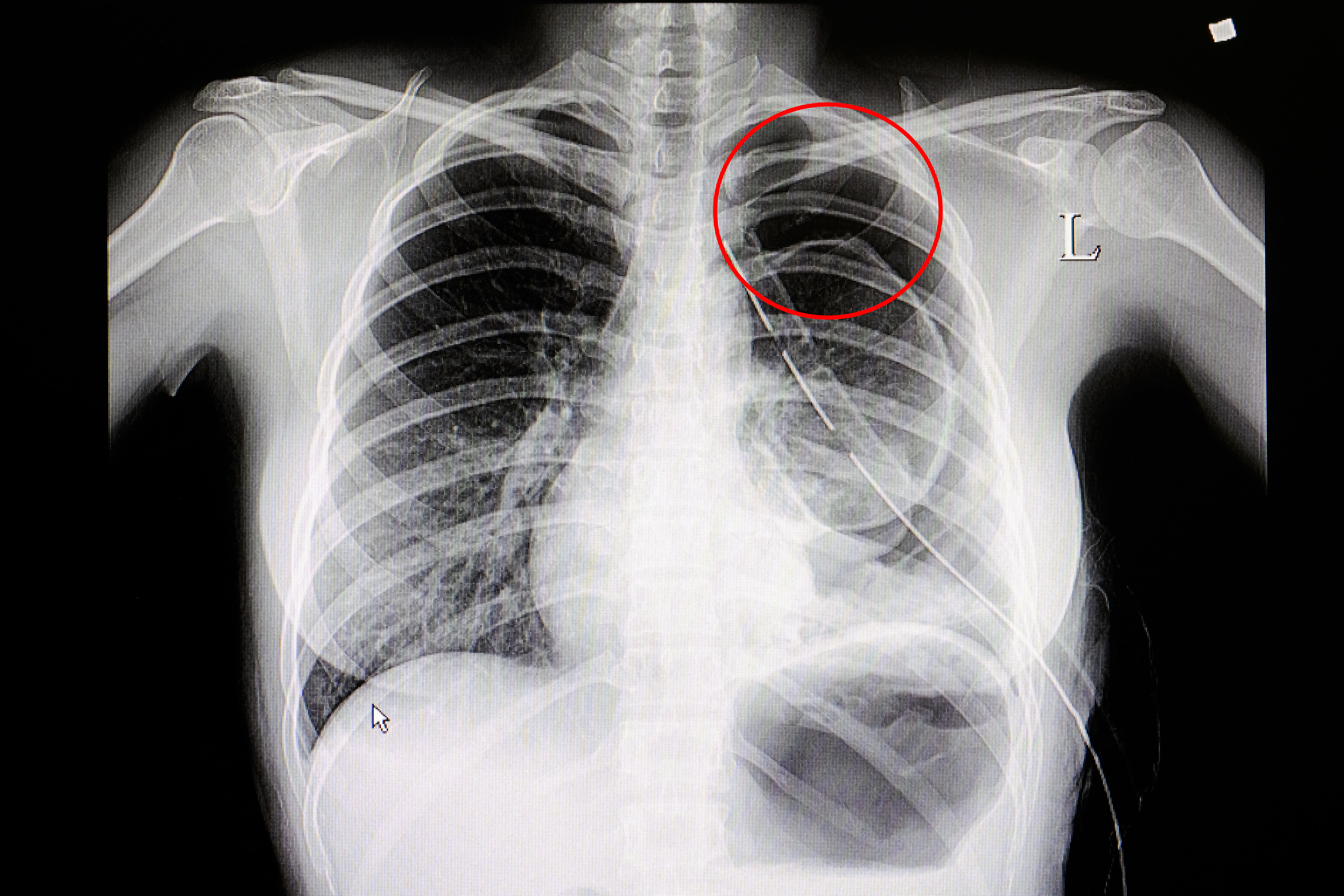
What Types of Pneumothorax Are There?
There are two basic types of pneumothorax: traumatic and nontraumatic. Traumatic pneumothorax is caused by physical injuries such as a fall, car accident, or any other type of injury that damages the chest or lung wall. Nontraumatic pneumothorax is also called spontaneous pneumothorax because it occurs without injury. There are many different factors that can contribute to or cause the onset of non-traumatic pneumothorax and it tends to be more difficult to understand than its counterpart.

There seem to be two separate instances where non-traumatic pneumothorax occurs and as a result, researchers have created two different classifications: primary and secondary spontaneous pneumothorax. Primary spontaneous pneumothorax (PSP) is more common in younger adults with no lung disease and secondary spontaneous pneumothorax (SSP) is more common in older adults with lung conditions.
One final classification that should be mentioned is spontaneous hemopneumothorax (SHP). This is an extremely rare but serious condition where both air and blood fill the pleural cavity, usually in patients who have no known history of chronic lung disease.
.jpg)
What Are the Symptoms of Pneumothorax?
Symptoms of pneumothorax vary based on what is causing the condition. Since pneumothorax can develop very slowly this may cause someone to underestimate the risk. However, in certain situations, it can develop very quickly causing someone to immediately seek medical attention. In mild cases, you may not experience any symptoms at all or at least not enough to cause you any concern. Below are some possible symptoms of pneumothorax:

- Dyspnea - shortness of breath
- Tachycardia - a fast heart rate
- Chest pain
- Cyanosis - a bluish discoloration of the skin
- Tightness in the chest
Causes and Risk Factors of Pneumothorax
Causes:
Mechanical ventilation - Mechanical ventilation is a medical procedure that’s used to assist someone with breathing if they are undergoing surgery or they have a medical condition that is preventing their lungs from working. While ventilation is mostly a safe procedure, if it is administered incorrectly and there is an imbalance of pressure within the chest, it can cause the lungs to completely collapse.
.jpg)
Ruptured air blisters - Small blisters called blebs can form on the top of the lungs in people with damaged lung tissue. Over time, these blisters can burst, allowing air into the pleural space. This can put a lot of pressure on the lungs and cause them to collapse.
Chest injury - Chest injury is a very common cause of pneumothorax. Blunt or penetrating injuries can occur during car accidents, sports injuries, or falls. Chest injury can also occur during lung surgery or it can be caused by collateral damage from other types of surgery.
Risk Factors:
Age - Pneumothorax is more likely to occur in young people between the ages of 20 and 40 or older adults with chronic lung conditions.
Gender - Tall underweight men are more likely to contract pneumothorax.
Smoking - Risk of pneumothorax increases with time and the number of cigarettes smoked.

Lung disease - Having a chronic lung condition like COPD, asthma, or cystic fibrosis puts you at a higher risk of pneumothorax.
Genetics - Studies have shown that mutations in the FLCN gene can cause pneumothorax.
Medical history - People who have experienced pneumothorax in the past are more likely to experience it again.
Why is COPD a Risk Factor for Pneumothorax?
The term chronic obstructive pulmonary disease (COPD) is an umbrella term used to describe two different diseases: chronic bronchitis and emphysema. Chronic bronchitis is characterized by inflammation in the bronchioles (bronchial tubes) which are the airways that lead to the lungs. Emphysema causes the alveoli (tiny air sacs in the lungs) to fill with fluid and impair the transfer of oxygen and carbon dioxide to and from the bloodstream.
One of the main reasons that COPD contributes to pneumothorax is because of the inflammation and damage that occurs to the lungs. While on the surface it may seem like COPD is a simple condition, it’s actually very complex and it affects the respiratory system in more ways than one. One thing that emphysema causes in particular are a change in the structure of the lungs. As the alveoli in the lungs start to break down, they lose their elasticity making it much more likely for air pockets to form in the pleural space.

Bullous emphysema results when fluid-filled sacs begin to form in the lungs. Bullae usually form in the upper lobes of the lungs and lung function can be significantly impaired if they become inflamed or rupture. This also weakens the overall structure of the lungs putting you at a higher risk of experiencing pneumothorax and other related issues.
In some cases, emphysema patients are a candidate for lung volume reduction surgery. While it may sound counterintuitive to reduce the size of the lungs of someone who can’t breathe well, this surgery is designed to remove only the diseased tissue. In other words, the surgeon will remove tissue that has lost its elasticity or isn’t able to transfer oxygen to the blood. This prevents the lungs from trapping air and allows you to breathe much easier.

Unfortunately, lung surgery can also be the cause of pneumothorax, especially if it involves a highly invasive procedure like lung volume reduction surgery. Before you decide that surgery is the best procedure for treating your emphysema, be sure to speak with your doctor about the risk of pneumothorax and ask any questions if you have them.
What Do COPD Patients Need to Do to Prevent Pneumothorax?
Schedule Regular Checkups
Probably the best thing you can do to prevent pneumothorax as a COPD patient is to see your doctor regularly. As aforementioned, pneumothorax isn’t always a condition that progresses quickly. In some cases, it can progress slowly and heal on its own. But to give yourself the best chance possible to recover quickly and effectively, you need to be aware of what’s causing it. Visiting your doctor regularly will give you a chance to discuss your symptoms and learn about your condition.

Follow Your Treatment Regime
There’s no doubt about it, you have a lot to worry about as a COPD patient. COPD treatment regimes usually involve a lot of different lifestyle changes like oxygen therapy, pulmonary rehabilitation, a revised diet, and an improved sleep schedule. While it’s not easy following all of these things to a tee, it’s worth it if you want to minimize your risk for common COPD complications like pneumothorax.

Quit Smoking Immediately
Smoking is the primary cause of COPD and it’s also one of the biggest risk factors for pneumothorax. So, it goes without saying that immediate smoking cessation will be hugely beneficial if you’re concerned about this complication. Smoking has been proven to increase the likelihood that a bleb will rupture which leads to air building up in the pleural space which collapses the lung.

Have an Action Plan
Another thing you can do is to simply have a plan in place in the event that you experience serious symptoms. Considering the fact that COPD exacerbations are a common occurrence you should already have an emergency plan in place. One thing you should do right away is to install a medical alert system in your home. The medical alert system comes with a small pendant that you wear around your neck. If you experience a medical emergency, simply press the button and an ambulance will be sent to your home.

How is Pneumothorax Treated?
Observation
The first thing your doctor will likely do if he/she suspects you have pneumothorax is to test for and observe your lungs. Chest X-rays and computerized tomography (CT) are the two most common tests used to detect but ultrasound imaging can also be used to get a better look at the lungs. If these tests reveal that you have a pneumothorax, your doctor may continue to observe it over the course of several weeks or months if it’s not urgent.
Needle Aspiration
This is one common treatment option for pneumothorax where a special needle is inserted into the pleural area. This needle extracts air so that the lungs can begin to re-expand and you can breathe normally again. Typically the needle is left in for several hours to ensure that all of the excess air is removed. A similar procedure is done by inserting a tube into the pleural space instead of a needle.
Nonsurgical Repair
If the above methods don’t work, there are several non-surgical options that your doctor might try. Bronchoscopy is a procedure that’s commonly used to examine the lungs and diagnose lung conditions, but in pneumothorax patients, it can be used to place a one-way valve in the affected area of the lungs. This will allow air into the lungs but prevent it from going back into the pleural area, thus re-expanding the lungs.
Surgery
If all other treatment options are exhausted, a medical specialist may resort to surgery in order to repair your pneumothorax. The specific type of surgery used to treat pneumothorax is called video-assisted thoracic surgery (VATS) or thoracoscopy. There are two other surgeries that can be done at the same time to prevent the resurgence of pneumothorax. These procedures are pleurodesis and bleb resection.
.jpg)
Pleural abrasion is one of the most common types of pleurodesis and it involves applying a special chemical designed to seal up the area of the lung that is leaking. Another way this can be done is by extracting blood from another area of the body and using this as a type of sealant to repair the leak. This is referred to as an autologous blood patch.
Conclusion
Pneumothorax, or a collapsed lung, is a scary thought regardless of whether you are a COPD patient or someone who’s otherwise healthy. In some cases, pneumothorax can be harmless and will heal itself over time. But in other cases, it can be life-threatening and require immediate emergency medical attention. Unfortunately, pneumothorax shares many symptoms in common with COPD exacerbations so it’s best to see your doctor any time that you experience a flare-up in your symptoms.
{{cta('43b79c5e-6bd6-4f02-ac27-2d038d20c146','justifycenter')}}
Here at LPT Medical, we are serious about providing COPD patients with reliable portable oxygen devices. While oxygen therapy will not prevent pneumothorax, it will ensure that you are able to use supplemental oxygen therapy wherever you go and reduce your risk of experiencing severe side-effects of COPD. Portable oxygen concentrators like the Caire FreeStyle Comfort and Inogen One G5 are our most popular units, but we offer many other options as well including pulse dose portable oxygen concentrators, continuous flow portable oxygen concentrators, and stationary oxygen concentrators.

