Pulmonary hypertension is a serious, chronic disease that affects the heart and the blood vessels in the lungs. Although it is somewhat rare, the disease can result from a large number of health conditions, genetics, or even occur spontaneously.
Unfortunately, most cases of pulmonary hypertension are chronic and incurable. But especially with early diagnosis and proper medical treatment, people with the disease are able to manage the symptoms of pulmonary hypertension and maintain a good quality of life.
In the early stages of the disease, people who have pulmonary hypertension tend to experience fatigue and shortness of breath during physical activity. But symptoms worsen and multiply as the disease progresses.
Life expectancy and treatment options depend mostly on how early the disease was caught and what cause, if any, doctors can find for the disease. In this guide, we will help you better understand pulmonary hypertension, what causes it, and what kind of treatments options are out there to help patients manage the disease.
{{cta('fa8abc2a-1e88-4fa3-82fd-1cb5b9ed43b2','justifycenter')}}
What is Pulmonary Hypertension?
Most people have heard the term hypertension, which is the name of a common condition where blood pressure is elevated throughout the body. Pulmonary hypertension is a bit different. It occurs when high blood pressure exists specifically in the blood vessels in lungs.
Pulmonary hypertension is somewhat difficult to define, because it can take so many forms and have so many causes. However, all forms of pulmonary hypertension affect the right ventricle of the heart, which is the chamber that pushes used (oxygen-depleted) blood out of the heart and into the lungs.
High blood pressure in the lungs happens when disease, inflammation, or other factors cause detrimental changes to the blood vessels in your lungs. These blood vessels, called pulmonary arteries, become thicker, stiffer, and the openings inside them get smaller.
These structural changes to the pulmonary arteries block blood flow and make it harder for your heart to continue pumping blood through your lungs. Thickened artery walls and inflammation make the inner space where blood flows narrower, causing hypertension and increasing the risk of blood clots.

Also, unlike healthy, flexible blood vessels, the thickened, stiffened artery walls found in people with pulmonary hypertension prevent the arteries from expanding to accommodate increased blood flow when needed. Basically, these changes in the pulmonary arteries work together to make the lungs a choke point for blood flow, raising blood pressure in the area and forcing your heart to work harder to push blood into your lungs.
Pulmonary hypertension is officially diagnosed by measuring blood pressure in the pulmonary arteries. If blood pressure in a lungs is greater than 25mm/Hg while at rest (or greater than 30 mm/Hg when exercising), the patient is said to have pulmonary hypertension. Healthy individuals have a resting pulmonary artery pressure between 8 and 20 mm/Hg.
How Pulmonary Hypertension Affects Your Body
To understand how pulmonary hypertension affects your body, you first have to understand the basics of how blood circulates through the heart and lungs. The following diagram of the heart and pulmonary arteries should help you follow along.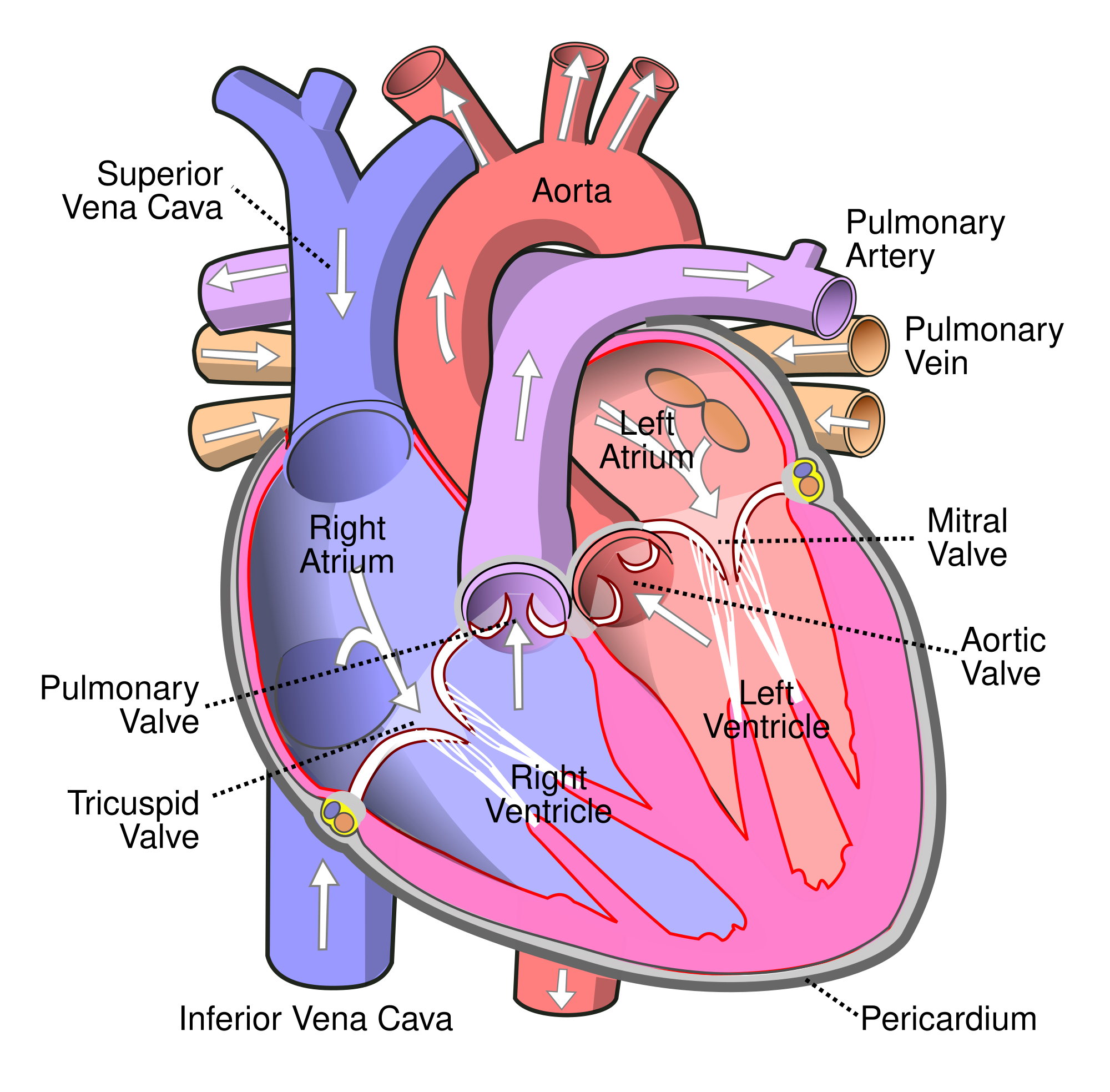
The heart is divided into two main sides: right and left. The heart is further divided from top to bottom, to make four heart chambers total.
The top two heart chambers are called ventricles, and they receive blood from other parts of the body. The bottom chambers are called ventricles, and they pump blood out to the rest of the body.
Pulmonary hypertension mainly effects the right ventricle (bottom right chamber) of the heart, which is responsible for pumping blood out of the heart and into the lungs. When the blood vessels in the lungs become stiff, narrow, or blocked, it creates back-pressure when the right ventricle tries to pump blood into the pulmonary arteries.
As a result, the blood pressure in the lungs goes up and the heart's right ventricle has to work harder and harder to push blood through the constricted arteries. Eventually, the resistance causes the right ventricle to enlarge and become weaker.
Over time, pulmonary hypertension causes the heart to continue to enlarge and get weaker and weaker, until it eventually is unable to pump blood into the lungs at all. The resulting heart failure is a major cause of death for people who are diagnosed with pulmonary hypertension.
This is the general mechanism by which pulmonary hypertension occurs and affects the body, but it is not the only one. There are several other forms of pulmonary hypertension that look slightly different and affect the body in different ways, which we'll discuss later in the section on causes of pulmonary hypertension.
Key Facts about Pulmonary Hypertension
Pulmonary hypertension is a rare and varied disease that has many different causes and can present itself in many different ways. In fact, there are five different groups of pulmonary hypertension, and within each of these groups there are multiple diseases and conditions that can cause a particular type of pulmonary hypertension.
It's estimated that only 15-50 people out of every million adults develops the disease, but the incidence is much higher for people in at-risk groups (including people with associated diseases like HIV or systemic sclerosis).
Idiopathic pulmonary hypertension (disease with no known cause) makes up more than 40% of total cases of pulmonary arterial hypertension. It is also, for unknown reasons, anywhere between 2 and 5 times more common in women than men, and is usually diagnosed around the age of 45 years.
In healthy people, the blood pressure in the lungs is significantly lower than the blood pressure throughout the whole-body, at about 8-20 mm/Hg. Unlike regular blood pressure measurement, testing the blood pressure in the pulmonary arteries requires special, more invasive techniques.
To test pulmonary artery pressure, doctors have to perform a procedure called right heart catheterization. It requires going under anesthesia and having a flexible tube, or catheter, inserted into a major blood vessel in your neck or groin.
The catheter is threaded up through the right side of the heart and into the pulmonary arteries. There it allows doctors to test the blood vessels in the lungs for high blood pressure and learn more about how efficiently your heart is able to circulate blood through your body. This is the most accurate way to test for pulmonary hypertension.
Pulmonary Hypertension Symptoms
In the early stages of the disease, many people who have pulmonary hypertension don't experience any major symptoms. It's one of the things that makes pulmonary hypertension so difficult to spot and diagnose.
When symptoms do show up, they usual begin slowly, starting with shortness of breath during physical activity. You might also notice minor chest pain, a racing pulse, and that you feel easily fatigued from minor physical activities.

Symptoms worsen slowly over time as the disease progresses and your body is unable to keep your blood oxygen levels up. You'll notice that even light activity can make you feel short of breath and experience light-headedness or even fainting. In the later stages, symptoms of severely low blood oxygen, such as a bluish tint to the skin and lips, and ankle or leg swelling (edema) can occur.
Here are some of the most common early symptoms of pulmonary hypertension:
- Shortness of breath (especially after light or moderate physical activity)
- Dizziness
- Racing pulse
- Heart palpitations
- Fatigue
- Reduced appetite
- Chest pain or pressure
- Pain in the upper-right side of the abdomen
Here are some of the most common later-stage symptoms of pulmonary hypertension:
- Feeling light-headed and dizzy
- Fainting
- Weakness
- Distended abdomen
- Bluish tint to skin and lips
- Swelling of the ankles and legs (edema)
Because pulmonary hypertension is a progressive, incurable disease, early detection is key. The longer it takes to get an accurate diagnosis, the worse the disease will become.
Many people, unfortunately, ignore or brush off the mild, early symptoms of pulmonary hypertension. Many others do go to see their doctor but are misdiagnosed with asthma or another type of lung disease.
The earlier you catch pulmonary hypertension, the more likely you are to be able to slow down it's progression with treatment and medication. That's why you should never ignore symptoms like breathlessness and fatigue, especially if you have a family history or other risk factors for pulmonary hypertension.
Causes of Pulmonary Hypertension
Pulmonary hypertension is a complex disease that affects the entire body and has many known causes. In some cases doctors are unable to find a cause, but in many cases pulmonary hypertension results from another known disease or health condition.
Different forms of hypertension affect the body in different ways, and what kind of treatment will be effective largely depends on what is causing the disease. That's why health researchers have divided up pulmonary hypertension into five main categories, each containing similar types of hypertension that are treated in similar ways.
The following sections describe the differences between all five categories of pulmonary hypertension and discusses the most common causes and conditions that lead to them.
Pulmonary Arterial Hypertension
This is a general form of pulmonary hypertension that includes forms caused by genetic mutations, viral infections, drug use, and certain medical conditions like heart and liver disease. It also includes forms of pulmonary hypertension that have no known cause (known as idiopathic pulmonary hypertension).
Pulmonary arterial hypertension occurs when the pulmonary arteries narrow and stiffen, causing high blood pressure in the lungs. This forces the heart's right ventricle to work harder, eventually causing it to enlarge and ultimately results in right-side heart failure.
Causes of Pulmonary Arterial Hypertension
- Heart Disease (including congenital heart diseases)
- Viral Infections
- Genetic Mutations
- Drug Use (especially amphetamines like cocaine or methamphetamine)
- Autoimmune Disease (including lupus, scleroderma, and rheumatoid arthritis)
- Chronic Liver Diseases (such as cirrhosis)
- Chronic lung diseases (such as emphysema, or pulmonary fibrosis)
- Unknown Cause (known as Idiopathic Pulmonary Arterial Hypertension)
Pulmonary Venous Hypertension
Pulmonary venous hypertension is different from pulmonary arterial hypertension in that originates from the left side of the heart. In this form of pulmonary hypertension, the left atrium (the upper-left chamber in the heart) has difficulty taking oxygenated blood out from the lungs.
As a result, excess blood pools up in the lungs because it cannot flow out of them efficiently. This creates back-pressure and makes it more difficult for the right ventricle to pump blood into the lungs, which results in pulmonary hypertension.
Pulmonary venous hypertension is often caused by problems and diseases that affect the left side of the heart, including connective tissue diseases that causes the heart chambers to narrow. It can also be caused by abnormalities in other parts of the heart, including problems that interfere with the ability of the heart valves to open and close correctly.
Causes of Pulmonary Venous Hypertension
- Left-sided Heart Disease (This is the most common cause of pulmonary hypertension)
- Left-ventricle Heart Failure
Hypoxic Pulmonary Hypertension

This category is referred to as hypoxic pulmonary hypertension because all of the diseases in the group share one major characteristic: hypoxia. The term hypoxia refers to lack of oxygen, and the condition occurs when blood oxygen levels are so low that all of the body's tissues are unable to get enough oxygen.
Lung diseases like interstitial lung disease or COPD, as well as sleep-related breathing disorders like sleep apnea, deprive the lungs of oxygen which can lead to hypoxic pulmonary hypertension. In these conditions, the lungs are unable to absorb enough oxygen, causing hypoxia in the lungs. This, in turn, causes many the blood vessels in the lungs to constrict, raising blood pressure in the pulmonary arteries.
Causes of Hypoxic Pulmonary Hypertension
- Chronic Obstructive Pulmonary Disease (COPD)
- Lung Diseases like Pulmonary Fibrosis
- Sleep-related breathing disorders like sleep apnea
- Exposure to high altitudes over long periods combined with other risk factors for pulmonary hypertension
Thromboembolic Pulmonary Hypertension
This type of pulmonary hypertension is caused by repeated instances of blood clots in the pulmonary arteries. It happens when blood clots get stuck in the small arteries in the lungs, restricting or blocking blood from flowing through.
In healthy individuals, blood clots usually don't get stuck in the lungs, or if they do, they resolve themselves without problem. But in rare cases where they don't dissolve or break up on their own, blood clots in the pulmonary arteries can result in pulmonary hypertension and right ventricle heart enlargement and failure.

Causes of Thromboembolic Pulmonary Hypertension
- Pulmonary emboli (chronic blood clots in the lungs)
- Medical conditions and procedures that carry a high risk of causing blood clots (This could include diseases that cause chronic inflammation, having your spleen removed, or having an infected pacemaker wire.)
Miscellaneous Pulmonary Hypertension
Miscellaneous pulmonary hypertension is basically a catch-all category for various forms of hypertension that don't fit into the other four categories. Most of the types of pulmonary hypertension in this category are caused by or related to other diseases and conditions, but the reason for the relationship is not well understood.
For example, certain metabolic disorders, connective tissue diseases, and HIV can lead to pulmonary hypertension, but doctors and researchers don't know exactly why this happens.
Causes of Miscellaneous Pulmonary Hypertension
-
Blood Diseases: Certain blood diseases, such as bone marrow disease, are associated with pulmonary hypertension. Doctors postulate that, because these blood diseases cause the body to produce excess red blood cells, they can contribute to pulmonary hypertension.
-
Systemic Disorders: Some systemic disorders cause a condition called vasculitis, a kind of inflammation that affects blood vessels throughout the body. Over time this can narrow blood vessels and restrict blood flow to vital organs and tissues, including the lungs, which can result in pulmonary hypertension.
-
Tumors: Certain conditions cause tumors to develop in the lungs or chest. These tumors can press against the pulmonary arteries, restricting blood flow and causing pulmonary hypertension.
- Metabolic Disorders: Some metabolic disorders, including thyroid disorders, Gaucher disease, and glycogen storage disease, can result in pulmonary hypertension.
Eisenmenger Syndrome: A Special Case of Pulmonary Hypertension
A type of congenital heart disease, Eisenmenger syndrome occurs most often when you have a large hole in the wall that separates either the two upper chambers in the heart (the left and right atria) or the two lower chambers of the heart (the left and right ventricle). A hole between the lower chambers is called a ventral septal defect.
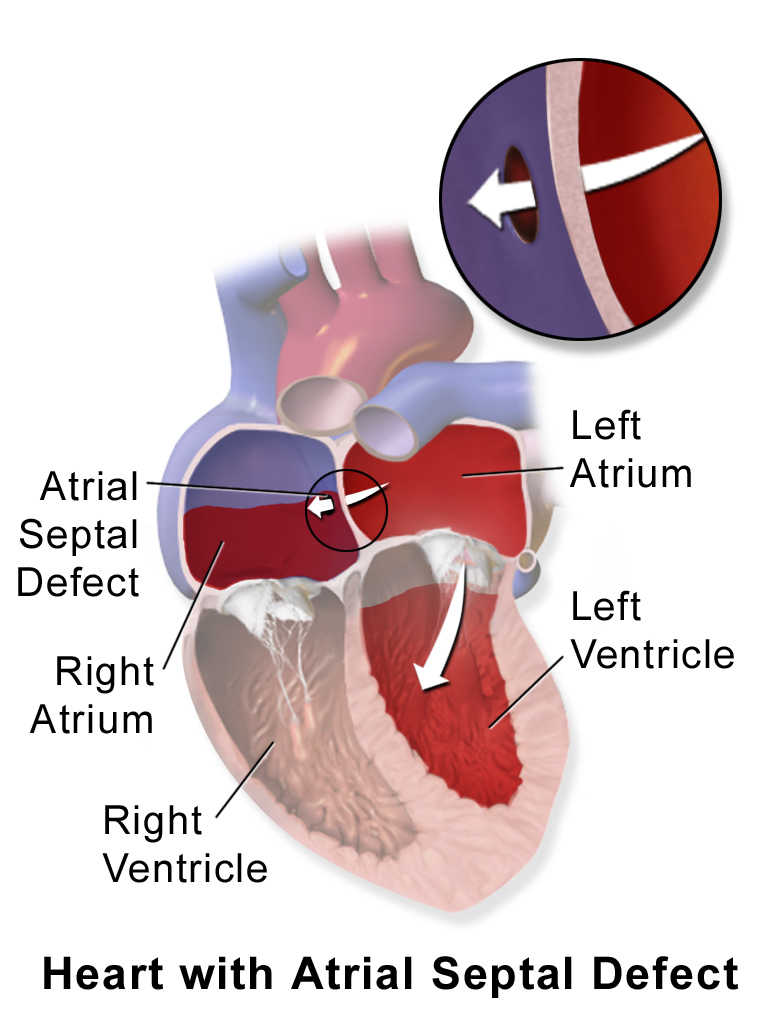
Because of this heart defect, blood cannot circulate normally, and blood in the two heart chambers gets mixed. This is a serious problem because the left ventricle is full of oxygen-rich blood that's ready to be pumped throughout the body, while the right ventricle holds oxygen-depleted blood that needs to be pumped through the lungs to get oxygenated.
This results in oxygen-poor blood being pumped through the body and oxygen-rich blood being needlessly pumped back through the lungs. This increases the volume of blood in the pulmonary arteries, which increases back-pressure, causes pulmonary hypertension, and eventually enlarges the lower heart chambers.
Complications with Pulmonary Hypertension
Pulmonary hypertension can lead to a variety of serious heart and lung conditions. Most of these complications occur later on as the disease progresses and puts increasing pressure on the right side of the heart.
Right-sided Heart Enlargement & Failure

Pulmonary hypertension causes back-pressure in the heart that causes it to have to work harder and harder to pump blood through the constricted pulmonary arteries. In order to compensate for the increased workload, the walls of the heart chamber thicken and the right ventricle expands and thickens (right ventral hypertrophy) so it can hold and pump more blood at a time.
However, these changes are only a temporary fix, and eventually the heart muscles weaken from the strain. Eventually, the right ventricle becomes so enlarged and weak that it fails completely, leading to right-sided heart failure and often death.
Blood Clots
In healthy people, small blood clots are usually able to pass through the lungs without causing any major problems. However, if you have pulmonary hypertension, the pulmonary arteries are narrowed, making blood clots much more likely to get caught and block blood flow in the tiny vessels.
Arrhythmia
Pulmonary hypertension causes your heart to enlarge and disrupts blood flow through the separate chambers. This can lead to irregular heartbeats, or arrhythmias, which can in some cases be fatal.
Arrhythmia can cause other dangerous and uncomfortable symptoms including faintness, dizziness, heart palpitations, and even fainting.
Bleeding
Bleeding into the lungs and coughing up blood is another serious, potentially fatal complication that can occur with pulmonary hypertension.
Risk Factors for Pulmonary Hypertension

Because the disease is so wide in scope, there are many potential risk factors for pulmonary hypertension. Along with the specific factors related to genetics, lifestyle, and medications, having any of the diseases or conditions known to cause pulmonary hypertension is a significant risk factor.
These are some of the risk factors that may increase your chances for developing pulmonary hypertension:
- A family history of pulmonary hypertension
- Being overweight
- Use of appetite-suppressant medications
- Illegal drug use (especially stimulants like cocaine and methamphetamine)
- Prolonged exposure to high altitudes
- Having any of the diseases or conditions that can cause pulmonary hypertension (listed in the section on pulmonary hypertension causes)
Treatments for Pulmonary Hypertension

Because many people with early-stage pulmonary hypertension only have mild symptoms, or even no symptoms at all, many people live with the disease for years before getting diagnosed. That's why it's so important to be able to recognize the early symptoms and get evaluated by a doctor if you notice them, especially if you're at a higher risk of getting the disease.
If the disease is caught early, proper treatment can delay the worsening of pulmonary hypertension and keep more serious symptoms at bay. However, no matter how long your disease has progressed, medication and lifestyle changes can alleviate symptoms and make a huge difference in your overall health and quality of life.
When you're diagnosed with pulmonary hypertension, the first thing your doctor will do is try to determine what caused you to get the disease in the first place. Different causes require different treatments, and you doctor will likely screen you for other diseases associated with pulmonary hypertension while searching for a cause.
If your doctor does find any underlying diseases or conditions that could be the cause of your pulmonary hypertension, your doctor will focus on treating those first. After those other conditions are treated and stabilized, your doctor will focus on medications and interventions to treat the pulmonary hypertension itself.
There are a variety of medicines, surgical procedures, and other treatments like supplemental oxygen therapy to help patients with pulmonary hypertension live longer, healthier, and fuller lives. Your doctor will work with you to create a personalized treatment plan and recommend the best course of action based on your unique case and medical history.
Lifestyle Changes
While lifestyle changes won't necessarily slow down the progression of pulmonary hypertension, they can improve your health and overall quality of life. Healthy habits can help you fight symptoms like breathlessness and fatigue and allow you to stay active in the later stages of the disease.
Stay Well-Rested

Getting enough sleep is an important part of any healthy lifestyle, but it's particularly important if you have pulmonary hypertension. The disease is taxing on your body and can make you feel tired and worn out, so make sure you take time to rest when you feel fatigued.
Quit Smoking
Along with increasing your risk for pulmonary hypertension, smoking causes further damage to your lungs and worsens symptoms of the disease. Quitting can be very hard, but there are many different programs, medications, and hot-lines available to help you if you need it.
Talk to your doctor about smoking cessation resources in your area or to get a prescription for a quit smoking medication. You can also visit the CDC's website for more information and support.
Eat Better
A healthy diet is key for good cardiovascular health