.png)
Headaches are a problem that we all deal with whether we’re young or old; healthy or not. A mild headache can detract from our daily life causing us to feel distracted, unmotivated, or restless. But at their worst, headaches can leave us completely unable to function in our daily lives. Many COPD patients may find themselves somewhere in between. You might get headaches periodically with varying degrees of severity, and experience periods of relief.
If you’ve noticed that you experience more headaches or more severe headaches since contracting COPD, the two conditions are most likely linked. In other words, focusing on treating your underlying COPD symptoms may help you to manage or completely eliminate your headaches as well.
{{cta('fa8abc2a-1e88-4fa3-82fd-1cb5b9ed43b2','justifycenter')}}
In the following article, we’ll take a look at some important steps you should take to treat headaches if you have COPD. As usual, if your headaches persist or you believe they may be caused by some other health issue, be sure to schedule an appointment with your doctor to discuss the potential cause.
How COPD Causes Headaches
Chronic obstructive pulmonary disease is a group of lung diseases that cause difficulty breathing. It’s called an “obstructive” disease because it makes it more difficult for a patient to expel air from the lungs. Diseases that make it more difficult for patients to inspire air are called “restrictive” because they’re caused by lungs that are unable to expand completely.
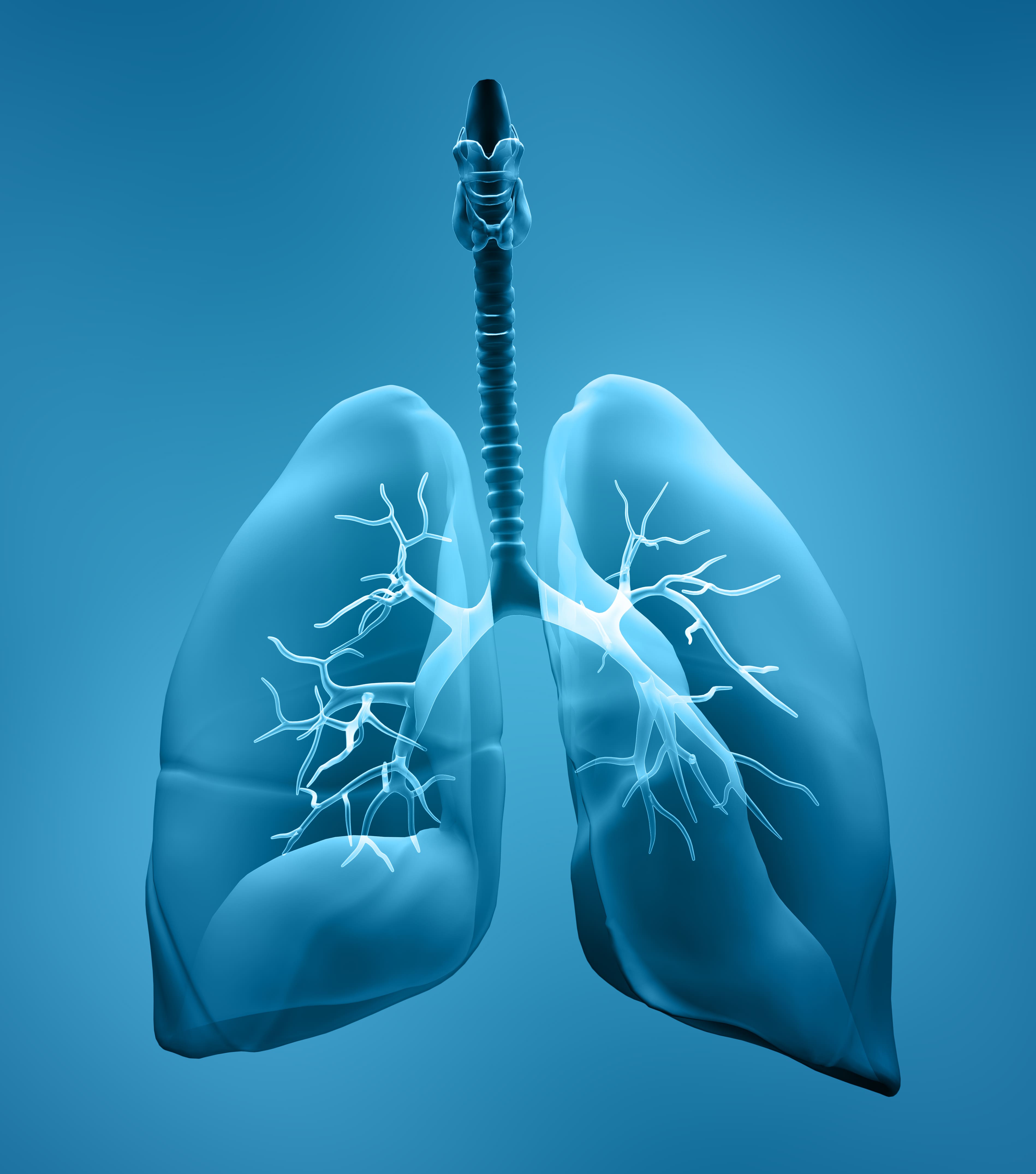
Your lungs have two functions: to bring in oxygen-rich air and to remove carbon dioxide-rich air. If one of these functions is out of balance, it can lead to a lot of problems. For example, hypoxia can occur when your blood has low oxygen levels. Over time, this can lead to severe symptoms, because your tissues are being deprived of a basic component that they need to function.
Another problem that can result from a chronic lung disease like COPD is hypercapnia. This is a condition that happens when you retain too much carbon dioxide. Having too much carbon dioxide in the blood can lead to similar symptoms as hypoxia by damaging organs and slowing the rate at which oxygen gets to your body’s tissues.
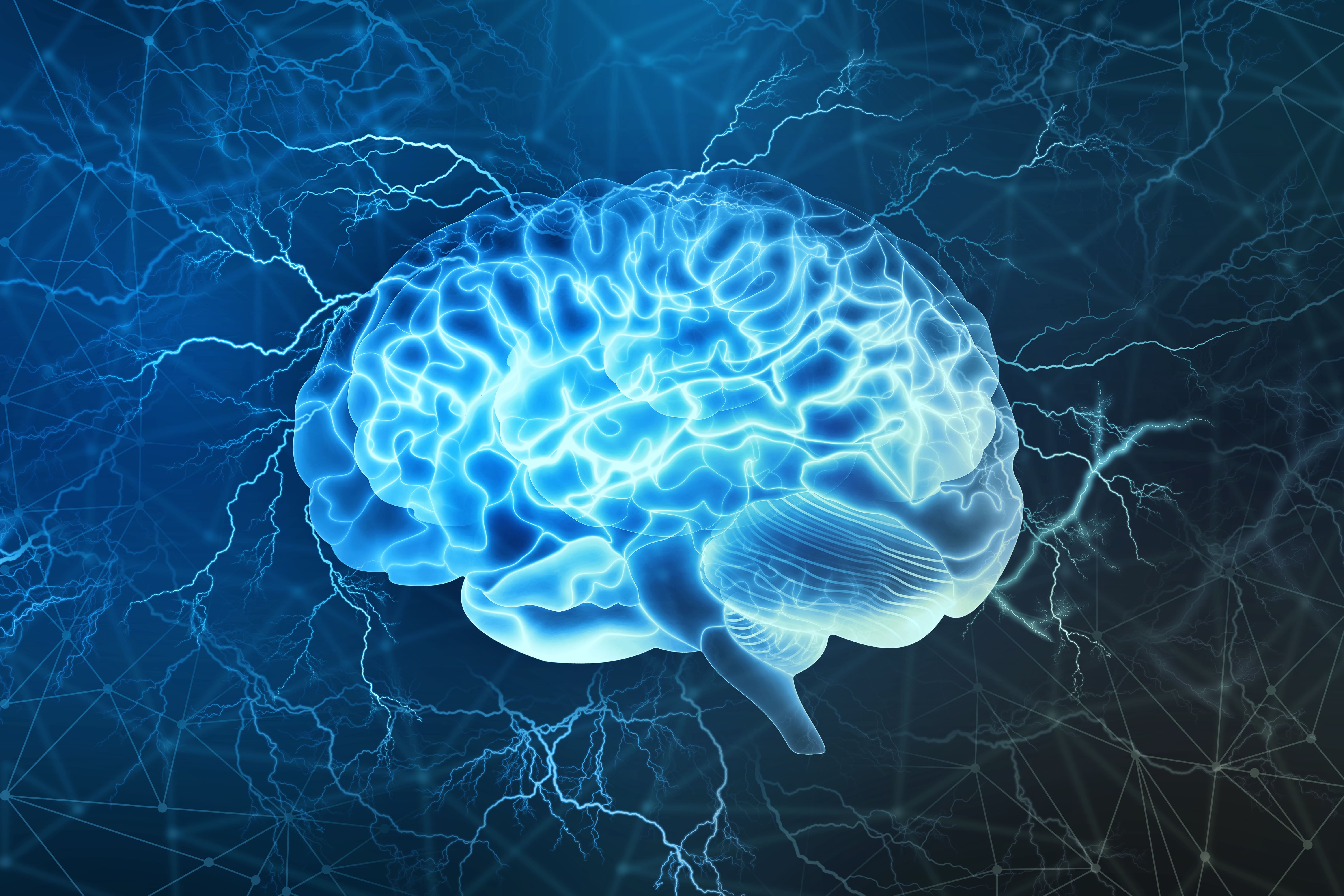
The most common cause of headaches in COPD patients is a low blood oxygen level due to either hypoxia or hypercapnia. While the brain only makes up about 2 percent of your body’s weight, it receives 15 to 20 percent of the body’s blood supply. As such, you’re likely to experience a headache due to low blood oxygen levels before any other symptom.
Many COPD patients experience headaches in the morning after waking up and this is likely due to sleeping problems such as sleep apnea which can be exacerbated by a chronic lung condition. When these two conditions occur together simultaneously, it’s called COPD-OSA overlap syndrome. If you have overlap syndrome, your doctor will likely prescribe both supplemental oxygen and CPAP or BiPAP therapy to help you sleep better at night.
Focus on Your COPD Treatment Plan
A COPD treatment plan is a set of steps you take to treat the underlying symptoms of COPD. Most doctors will recommend some combination of supplemental oxygen therapy, pulmonary rehabilitation, an improved diet, and a revised sleep schedule. However, depending on the severity of your COPD and whether or not you have comorbidities may affect how you should be treating your disease.

The reason that you should start with your treatment plan is that it will rule out COPD as the cause of your headaches. If you’re doing everything that you should be doing to manage your respiratory health and you’re still experiencing headaches regularly, it’s safe to say that there is something else causing the issue. On the other hand, if you’re experiencing headaches in the morning, they could be due to a drop in blood oxygen levels at night. In this case, you may need to talk to your doctor about having a sleep test done.
Supplemental Oxygen Therapy
The vast majority of people with COPD are prescribed supplemental oxygen. Some people are only required to use it several hours a day or as needed when blood oxygen levels are low. However, a large number of COPD patients need to use oxygen for 16 hours or more each day. Unfortunately, some people find themselves either falling back on the supplemental oxygen plan their doctor set for them or they are unknowingly using their oxygen device incorrectly.

Oxygen tanks have been the industry standard for oxygen therapy for a long time. But they don’t meet the needs of every oxygen patient because they’re heavy and bulky. As a result, oxygen tank users frequently feel like they aren’t able to get where they need to go without help from a friend or loved one. Carrying around a heavy oxygen tank can also lead to breathlessness, low blood oxygen levels, and thus headaches, so it may be worth it to look for a different oxygen therapy device.
Portable oxygen concentrators offer a much more convenient way to use oxygen. Since they’re both small and lightweight, they help you ensure that your oxygen needs are met wherever you go. POCs are battery-powered, so you’ll never find yourself where you run out of oxygen. Simply plug it into any car or wall outlet and you can continue using it and charging your batteries.
Pulmonary Rehabilitation
Pulmonary rehabilitation is a fancy way of saying exercise that’s focused on your lung health. Pulmonary rehab is a supervised program meaning you will work with a medical expert who will show you the proper way to exercise if you have impaired lung function. However, once you know how to exercise correctly, you can perform pulmonary rehabilitation in the comfort of your own home.

The reason pulmonary rehab is so important in preventing headaches is that a sedentary lifestyle and poor posture can make you more susceptible to headaches. Consistent moderate exercise is one of the best remedies for headaches because it keeps blood flowing to the brain and the rest of the body. Exercise also helps you improve your posture which is another thing that can affect your body’s circulation.
{{cta('b59df0c1-c4de-47a8-8e1c-0d33d4b414aa','justifycenter')}}
Healthy Diet
Your diet plays an immense role in your body’s ability to ward off headaches. According to migrainetrust.org, skipping meals, dieting, eating high-sugar foods, and fasting can all contribute to or cause headaches. What’s more, according to COPD News Today, studies suggest that inflammation caused by COPD can contribute to the development of type 2 diabetes. This condition is known for causing low blood sugar (hypoglycemia) and as a result, headaches.

As a COPD patient, your diet should be strictly regulated. First and foremost, you should be eating smaller meals throughout the day rather than one or two big meals. Your body may struggle to digest larger meals, so the more you can spread out your meals, the better. Secondly, you need to be eating the right types of foods. COPD patients need food that is high in fiber, protein, and healthy fats, but low in added sugar and salt, as well as highly processed or fried foods. This will ensure that your lungs remain healthy and strong and you don’t have any bouts of hunger or energy loss that could lead to headaches.
Smoking Cessation
Smoking is likely one of the most common causes of headaches in COPD patients. According to the Centers for Disease Control and Prevention (CDC), 38% of COPD patients are current smokers. While smoking temporarily alleviates stress, anxiety, and headaches, the withdrawals you experience after the fact can be particularly painful. According to WebMD, insomnia, cravings, and headaches due to nicotine withdrawal typically begin 3 to 5 days after you last smoked. If you’re trying to quit smoking but keep falling back on your plans, this could be why you’re experiencing headaches.

Avoid COPD Triggers
A COPD trigger is anything that can cause a flareup in your COPD symptoms. Some common COPD triggers include cigarette smoke, car exhaust, indoor cleaners, dust, pollen, and more. COPD triggers can cause your airways to constrict, increase inflammation in the lungs, and increase the production of mucus, all of which make it more difficult to breathe. Additionally, COPD exacerbations can lead to a high degree of stress and anxiety, all of which can contribute to headaches.
![]()
Ideally, you should be conscious of the quality of air that you are breathing throughout the day. When you’re indoors, make sure you are not exposed to dust, mold, or toxic cleaning supplies. And before going outside, be sure to check the air quality index to make sure the air is clean enough for someone with a chronic respiratory illness. Also, be sure to have a plan for dealing with flare-ups and exacerbations.
Drink Lots of Water
According to the H.H. Mitchell, Journal of Biological Chemistry, the heart and brain are composed of 73% water and the lungs are composed of 83 percent water. What this means is that depriving your body of water doesn’t just prevent your brain from getting the water it needs, but it also makes it more difficult for your heart and lungs to bring oxygen-rich blood to your brain. While every tissue in your body needs water, your brain needs it most of all.
.jpg)
COPD Medications
The medications that you take for COPD can be both the cause of, and the cure for your headaches. Generally speaking, taking medication as it’s prescribed by your doctor will help stabilize your blood oxygen level and mitigate the chance that you will experience an exacerbation or other COPD-related complication. However, some COPD medications have “headaches” listed as a side-effect, so this isn’t something you should rule out.

Fast-acting bronchodilators (also known as rescue inhalers) are an important part of any COPD treatment plan. They include drugs like albuterol, albuterol sulfate, and levalbuterol, and they’re responsible for quickly alleviating COPD symptoms like chest tightness and excess mucus production. However, fast-acting bronchodilators are also known for having a lot of side-effects like headaches, dizziness, and nausea.
Be Careful With Pain-Relief Medications
Unfortunately, most discussions around COPD are focused on alleviating the symptoms of the disease and less on alleviating pain that’s associated with those symptoms. While pain medication can be used safely and effectively in COPD patients, it should not be seen as a cure-all or something that’s used on a daily basis. What’s more, you have to be careful about what pain relievers you’re using and how they will interact with your COPD medications.
Consult Your Doctor
While you can continue to research the potential cause of your headaches, the best way to deal with this problem as quickly as possible is to consult your doctor. While it may seem like a hassle to go to the doctor just to ask about your headaches, there could be a very simple solution to your problem or there may be a more serious underlying problem that your doctor needs to know about. Be sure to write down the following information before you schedule an appointment:

- The frequency and severity of your headaches
- What time of day or night your headaches occur
- The location on your head that you feel the most pain
- What foods you’re eating each day
- How much water you’re consuming daily
- What your sleep schedule is like
- Any additional medication you’re taking (that wasn’t prescribed by your doctor)
Conclusion
Headaches are not an uncommon side-effect of chronic obstructive pulmonary disease. Likely one of the first symptoms you will experience if your blood oxygen levels are low is a headache. But there’s also a chance that the pain you’re experiencing is completely unrelated to your respiratory condition.
Start by trying a few of the tips listed above and if they don’t work, be sure to consult your doctor. While there may be a simple solution to your headache problem, they could be a sign of a more serious underlying condition, so it’s best to speak with your doctor sooner rather than later.
In the meantime, if you’re looking for a new mobile oxygen machine to manage your respiratory condition, feel free to browse our portable oxygen concentrators here at LPT Medical. We offer all of the most popular and reliable units including but not limited to the Caire FreeStyle Comfort and the Inogen One G5. Both of which weigh under 5 pounds and offer outstanding battery life to keep you out and about for longer. Speak with one of our respiratory specialists to learn more.

